Understanding Appendicitis
What is the Appendix?
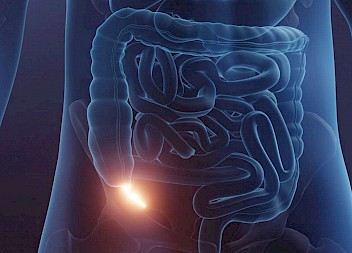
The appendix is a (worm-like) continuation of the large intestine found at the junction of the small and large bowel. It is a vestigial organ, and its existing function in the human body is still unknown.
What is Appendicitis?
Appendicitis is the painful swelling or inflammation of the appendix. It typically results when it is blocked by stool, foreign body or cancer, resulting in the growth of bacteria, inflammation and pain. Appendicitis can affect people of all ages, but peak incidence occurs for those aged between 10-30 years old.
An inflamed appendix is often a prelude to an appendix bursting or perforating, causing infectious materials to be released into the abdominal cavity. This can lead to peritonitis, a serious inflammation of the abdominal cavity’s lining (the peritoneum) that can be fatal unless it is treated quickly with broad-spectrum antibiotics.
Sometimes a pus-filled cavity (an infection that is walled off from the rest of the body) develops outside the inflamed appendix. An abscessed appendix can explode or perforate, causing peritonitis.
What are the symptoms of Appendicitis?
The typical pain starts in the navel region and shifts towards the lower-right side of your abdomen.
- Pain in the right lower quadrant of the abdomen
- Pain is aggravated by coughing, walking or making other jarring movements
- Loss of appetite
- Nausea and vomiting soon after abdominal pain begins
- Swollen belly
- Fever of 99-102 degrees
More severe symptoms like when a patient cannot pass gas indicate obstruction, which can quickly cause perforation of in the intestines. It is crucial that the medical practitioner recognise these symptoms early in the course of managing the patient so that life-threatening complications can be avoided.
What tests are used to diagnose appendicitis?
- Physical examination of the patient showing rebound tenderness and other signs of appendicitis
- Blood tests to see markers of inflammation, white cell count and other elements that constitute the diagnostic criteria
- Abdominal X-ray
- An Abdominal CT-Scan remains gold-standard for diagnosis of appendicitis.
Do You Have a Claim?
Why is it common to misdiagnose appendicitis?
Unfortunately, the signs and symptoms of appendicitis are not always consistent or specific; thus, leading to misdiagnosis, frequently causing medical negligence claims.
Appendicitis does not always present with typical symptoms. Instead, it mimics other minor conditions affecting the abdomen. Appendicitis can be confused with a range of other disorders like gastroenteritis, constipation, severe irritable syndrome (IBS), urine and bladder infections, Crohn’s disease and, for women, menstrual pain and ectopic pregnancy. However, this is not to say that medical practitioners may be exempted for failing to make a timely diagnosis. Instead, it is their duty to ensure that the correct diagnosis is obtained at the right time.
While in some cases a diagnosis may be difficult because the condition is at too early a stage or the symptoms are not ‘specific’, we frequently see cases where appendicitis has been missed by medical practitioners, despite the patient’s history and clinical examinations which strongly indicate its presence.
Complications that result in negligence claims
Around 40,000 patients are admitted to hospital with appendicitis in England every year. Delays in treatment can result in complications, a protracted recovery, with financial consequences and – in rare cases – death.
Delayed Diagnosis resulting in infection before or after surgery. If you are not given a timely diagnosis, then your appendix may rupture, releasing faecal matter in your abdomen, causing massive infection. Every medical practitioner owes their patient a duty of care to ensure that they are not harmed by their negligence. Infection claims may arise if a patient was not prescribed the correct medication or if they contracted a hospital-acquired infection.
Perforation or Rupture due to delayed treatment. This occurs due to a delay in diagnosis. The risk of perforation is 15% within the first 36 hours of the onset of symptoms. This means that if your doctor failed to diagnose your symptoms within 36 hours due to negligence, then the most-feared complication of appendicitis – perforation can result. Perforation of the appendix can result in:
- an abscess (a collection of infected pus), or
- diffuse peritonitis (inflammation of the entire lining of the abdomen).
The major cause of appendix perforation is a delay in diagnosis and treatment. Generally, the extensive the delay between diagnosis and surgery, the more likely a perforation results. Thus, once appendicitis is diagnosed, surgery should be performed without unnecessary delay.
Blockage of the intestine. Blockage occurs when the inflammation around the appendix involves intestinal muscle and makes them paralysed, or there is physical obstruction from the contents of the inflammation. Intestinal obstruction can be readily suspected in a patient who isn’t able to pass flatus and should be immediately sent for abdominal decompression to avoid perforation.
Life-threatening complication – sepsis: It results when the infecting bacteria enter the bloodstream and travel to other parts of the body. This is a severe, even life-threatening complication which needs to diagnosed and managed appropriately. Fortunately, it occurs infrequently.
Infertility due to Inflammation: the inflammation that results from bursting of the inflamed appendix can involve several organs, including the fallopian tubes in females. The resulting scarring and adhesions cause blockage of the tubes, thereby preventing the sperm to reach the eggs. This prevents pregnancy in the affected females. As unfortunate as it sounds, this is a reversible form of infertility and in some cases can be successfully managed with IVF.