Ovarian cancer is the gynaecological cancer with the most fatal outcome, killing more women than the other four gynae cancers combined.
Around 4,000 women in the UK die from ovarian cancer every year. Two thirds of these die needlessly, having been diagnosed at later stages when the chance of cure is poor. Why is that?
Ovarian cancer has historically been called the silent killer, as many believe the symptoms are undetectable until the cancer has progressed. Better recognition of symptoms by both clinicians and patients would identify ovarian cancer earlier, improving the outcome for patients diagnosed with the disease.
Early symptoms of ovarian cancer can be confused with other health complaints.
One of the main reasons why ovarian cancer is diagnosed late is because the early symptoms mimic those of other conditions. Warning signs of ovarian cancer are generally misdiagnosed as bowel problems like IBS, or mental health disorders like stress and depression.
Women have been conditioned to accept abdominal pain as normal. Many women with ovarian cancer are diagnosed after presenting at emergency departments with excruciating pain, having exhausted all other options of primary care without any answers. It can be tricky as a patient to know when to challenge medical advice you’ve been given. But all patients, no matter their gender, need to be given the opportunity to express themselves, and be listened to, if they believe something isn’t right.
There is no reliable screening programme for ovarian cancer in the UK. We do have a very good cervical screening programme but this doesn’t detect ovarian cancer.
That’s why it is important to know just what symptoms to look out for and seek medical advice if you frequently have any of them – that being around 12 times or more a month.
What are the symptoms of ovarian cancer?
- Bloating
- Pain in tummy or pelvis
- Feeling full quickly after eating
- Loss of appetite
- Frequent or urgent need to urinate
- Indigestion
- Constipation or diarrhoea
- Back pain
- Losing weight unintentionally
- Vaginal bleeding post-menopause
More information about symptoms and how to track them can be found on the Ovacome website.
What is ovarian cancer?
Ovarian cancer is one of the five gynaecological cancers. It affects the ovaries which are the two small organs in the reproductive system where eggs are stored. It mainly affects women after the menopause and is rare in women under 40, but that doesn’t mean you can’t get ovarian cancer when young.
What are the causes of ovarian cancer?
The causes of ovarian cancer are largely unknown. There are however some factors than can put people at higher risk.
You may have an increased risk of ovarian cancer if someone in your close family has had ovarian, breast or prostate cancer. Also, your risk increases if you have the BRCA1 or BRCA2 gene mutation.
Ovulation is thought to contribute to the development of ovarian cancer, as the ovary’s DNA is damaged each time ovulation occurs. If you started your periods early, went into the menopause late, or haven’t been pregnant, you might have an increased risk of ovarian cancer as you will have ovulated more over the years.
Women with endometriosis or diabetes may also have an increased risk, as too do those who are overweight or smoke.
How is ovarian cancer detected?
If you believe you have symptoms of ovarian cancer, you should see your GP who will do an internal vaginal examination and arrange some initial tests. These include a blood test which measures your CA125 level, a protein that may indicate you have ovarian cancer if levels are raised, and an internal or abdominal ultrasound scan.
If these tests are abnormal, your GP will refer you to see a specialist in gynaecological cancer under the two-week cancer pathway. The specialist doctor may arrange further tests including a CT scan, biopsy, or laparoscopy to help make a diagnosis. Receiving a diagnosis of ovarian cancer may cause you to feel anxious and your specialist team will usually include a specialist nurse to whom you can turn for support and to answer your questions.
You will usually undergo further tests to find out more about the size of the cancer and how much it has spread such as a CT scan, MRI scan, and PET scan. Genetic testing may be offered.
How is ovarian cancer treated?
Treatment offered will depend on the size and type of ovarian cancer, where it is, if it has spread, and your general health. Usually, the cancer is removed by surgery followed by chemotherapy. You may be offered hormone treatment and medication.
You will have a higher chance of survival if surgical removal is possible, and the cancer has not spread outside the ovaries, which is why early detection is crucial.
What are the stages of ovarian cancer?
Stage 1 - the earliest stage, affecting only one or both of the ovaries, or one or both fallopian tubes. 1 in 5 people diagnosed at this stage. The outcome is generally good, especially if contained to one/both ovaries.
Stage 2 – cancer has spread to the pelvis or womb. Only found in small number of people.
Stage 3 – cancer has spread beyond the pelvis into the abdominal cavity or to lymph nodes. The most common stage at which ovarian cancer is diagnosed.
Stage 4 – cancer has spread beyond the abdomen to other organs such as the liver or lungs.
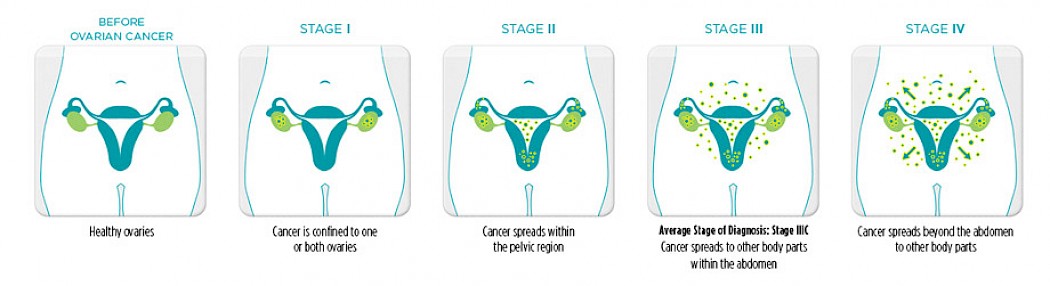
Credit: Physiopedia.com
Can I bring an ovarian cancer medical negligence claim?
Delayed diagnosis is one of the main reasons why someone would bring a medical negligence claim for ovarian cancer. Patients who have experienced delays in diagnosis have usually experienced more invasive treatment that may not have been necessary, had the cancer been found earlier. In addition, a patient’s chances of survival may have been affected.
Other issues relating to ovarian cancer medical negligence include:
- Abnormal tests not followed up
- Incorrect reporting of tests
- Failure to examine a patient experiencing symptoms
- Failure by a GP to refer a patient with symptoms to a specialist
- Symptoms repeatedly misdiagnosed as another condition
- Substandard treatment or care during surgery
What might compensation cover in ovarian cancer medical negligence claims?
Women who have both ovaries removed during treatment, and have not yet entered the menopause naturally, will go into surgical menopause. Chemotherapy can also induce menopause. If the patient is still in their childbearing years, this will obviously affect fertility.
We have acted in cases previously where we have successfully recovered the costs of surrogacy abroad to enable a client to expand their family, in circumstances where they are unable to child-bear themselves, owing to medical negligence.
Cancer treatment can impact a person’s ability to work, adding further financial strain to a family. Compensation can cover any future care or treatment costs you may need, as well as reimburse you for any past or future financial losses resulting from your experience.
Will making a medical negligence claim affect future cancer treatment?
Many people believe this may impact their future treatment for the cancer. But it is unlawful for any medical professional to withdraw treatment due to a claim being made against them.
Our team of specialist medical negligence solicitors have supported many clients who have experienced delayed diagnosis of cancer. We understand that these clients and their families are living through challenging times with lots of questions they want answering as to why their concerns weren’t listened to or why their care fell short of the expected standard.
If you have questions about a possible ovarian cancer medical negligence claim, our friendly team are here to listen. After an initial chat, we can request your medical records and advise whether you do indeed have a medical negligence claim.
Medical Solicitors works on a No Win No Fee basis, so you have nothing to lose by making an initial enquiry.
Please Note: At Medical Solicitors, our team specialise in handling delayed diagnosis claims involving healthcare providers in England and Wales and will be happy to extend a helping hand if your case is located in either of these regions. Unfortunately, we do not manage delayed diagnosis claims outside of England and Wales.

